
LATEST NEWS

Judge Tosses Blakeman’s Attempt To Block Attorney General’s Order

Carle Place Students Experiment In DNA Lab

Floral Park-Bellerose School Students Perform At Orchestra Festival

Westbury’s Techno Dragons Win Big For Innovative App

Snapshots Of Easter Weekend From Our Neighbors

Mineola Chamber Hosts Local Leaders At February Dinner
Virtual Reality Project Earns Second NEH Grant

Cradle Of Aviation Shines On Eclipse Day
Cradle of Aviation Museum held a unique educational event celebrating the solar eclipse on Monday, April 8. The museum staff used the rare natural phenomenon

Blakeman, LaRocco Recruit Locals To Deputize In Emergencies
Nassau County Executive Bruce Blakeman is back in the news this spring after putting out a call for new Nassau County Provisional Special Deputy Sheriffs,
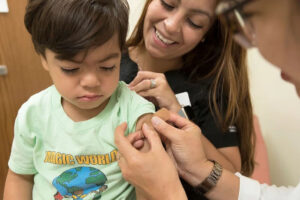
Measles Case In Nassau Renews Calls For Vaccination, Education
In late March, a young child who presented with symptoms at a Nassau County emergency room was confirmed to have measles, prompting renewed attention to

Hillside Islamic Center Files Suit Over Construction Plans
After months of consideration and back-and-forth discussion, the Town of North Hempstead’s town board recently voted against a revised proposal by the Hillside Islamic Center

Westbury’s Techno Dragons Win Big For Innovative App
The fourth- and fifth-graders of Park Avenue School’s Techno Dragons have been working hard this year to get their FIRST LEGO League (FLL) robotics and

Irish American Society Hosts 74th Successful St. Patrick’s Day Parade
Irish eyes were smiling when the sun shined bright on the annual St. Patrick’s Day parade in Mineola on Saturday, March 3. The Irish American
TRENDING
(Photo from NBCUniversal)
Chuck Scarborough:
A Beacon of Journalistic
Longevity
By Christy Hinko • April 22, 2024
THIS WEEK'S
SPECIAL SECTIONS

UPCOMING EVENTS
- Check back for future events



